Publication
This case report was published in PPD journal. Click here for full article.
Case report
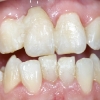
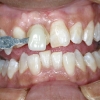
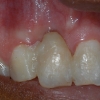 This case report emphasizes the importance of site development and provisionalization in achieving optimal results in the aesthetic zone. The patient presented with a chief complaint of poor aesthetics from loss of tooth #8. His dentist extracted tooth #8 and placed a bonded provisional restoration. No grafting was performed. He was initially told he does not have enough bone and was advised to get a fixed bridge. However, the patient was hesitant to follow this recommendation and sought a second opinion.
This case report emphasizes the importance of site development and provisionalization in achieving optimal results in the aesthetic zone. The patient presented with a chief complaint of poor aesthetics from loss of tooth #8. His dentist extracted tooth #8 and placed a bonded provisional restoration. No grafting was performed. He was initially told he does not have enough bone and was advised to get a fixed bridge. However, the patient was hesitant to follow this recommendation and sought a second opinion.
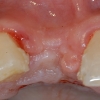
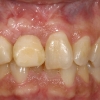
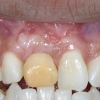
The extraction site showed horizontal atrophy as well as mild vertical atrophy. The adjacent teeth had healthy periodontal apparatus; however there was gingival disharmony due to loss of tissue.
Treatment
1. Patient initially seen by the restorative dentist, Dr. Watkins, for provisionalization of tooth #8. The provisional restoration provided some guideline for the final result as well as degree of tissue deficiency.
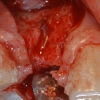
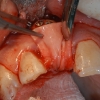
2. The first surgical phase consisted of bone augmentation. This was accomplished with an onlay graft in combination with a particulate graft and GTR membrane to enhance horizontal bone and vertical dimension as much as possible. Bone was harvested from the ramus area. A transitional prosthesis was used during the healing period.
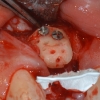
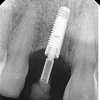
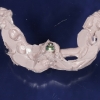
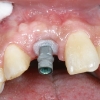
3. Six months later, an implant was placed using a surgical guide prepared from a complete wax up. This is a critical step in accurate placement of the implant in all vectors. Connective tissue graft was also done to develop further soft tissue on the labial aspect.
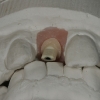
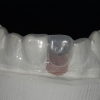
4. Following 3 months of healing, the implant was exposed, a healing abutment placed, and provisonalization was begun immediately to the soft tissue design. A proper provisional restoration with correct dimensions is an integral part of tissue harmony and aesthetics.
5. After three months of provisionalization, a new implant level impression was obtained. At this time, the gingival tissue was thick and quite stable and further remodeling was not expected.
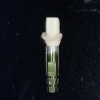
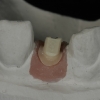
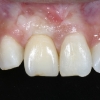
6. Lastly, a ceramic abutment and crown were fabricated and placed.
Success factors
1. The diagnostic work up began with the end in mind.
2. There was adequate bone and soft tissue augmentation.
3. A proper surgical guide allowed accurate placement of the implant.
4. Proper provisional restoration was completed.
5. The surgeon and restorative dentist worked in collaboration, each doing what they do best.
6. The patient physiology of healing aligned with the proposed treatment.