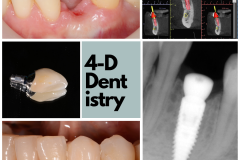
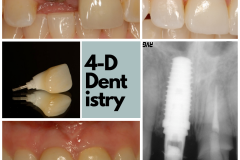
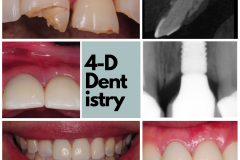
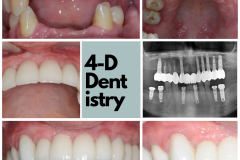
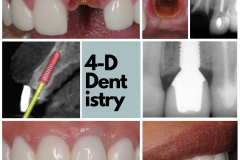
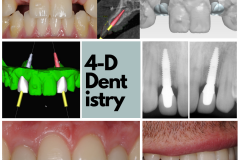
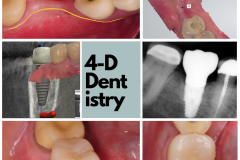
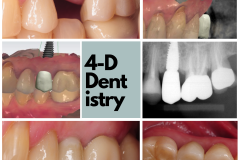
 To me, losing a tooth is a big deal. I’ve had nightmares about teeth falling out of my mouth! I wake up in a desperate panic and experience an overwhelming sense of relief when I realize that it was just a bad dream. But, what really happens when a person loses a tooth?
To me, losing a tooth is a big deal. I’ve had nightmares about teeth falling out of my mouth! I wake up in a desperate panic and experience an overwhelming sense of relief when I realize that it was just a bad dream. But, what really happens when a person loses a tooth?
Well, there are actually three things that happen:
First, of course, the very obvious—it looks bad. A big dark hole, which for many is very traumatic. And the temporary flipper makes it even worse. Now the person has to live with a plastic removable partial denture which not only looks fake but also feels awkward at best. The person also loses their chewing balance, so they try to avoid the empty space by chewing on the other side. I’ve never had a missing tooth, but I hear it’s a strange feeling when you are trying to chew, and the food just slips by your other teeth and hits the gum tissue in the space where a tooth used to be.
Second, there are the structural changes—the thinning bone and gum tissue that follows. Also, adjacent teeth may start moving and/or experience overload that can lead to further compromise given enough time.
Third is the emotional impact, which is often more significant than the physical changes. Depending on the location of the missing tooth, the person may feel self-conscious and embarrassed and, consciously or unconsciously, avoid smiling or laughing—not being able to fully experience one of the most pleasurable expressions—smiling. The person may feel deficient, imbalanced, or perhaps even handicapped to some degree. A sense of loss and even grief may be felt as they try to come to terms with the fact that part of their body is no longer there.
So, it’s no small thing to lose a tooth. It affects a person on so many levels. And, for many, the experience is devastating enough that they are willing to invest lots of time and money to feel “normal” again. That’s where we—the dentists—can help. We now have the opportunity and the responsibility to give the person back everything that has been lost.
That’s a big responsibility! We have to restore what has been lost—the missing bone, the missing gum tissue, the missing chewing ability, the missing smile, the missing confidence, and the missing feeling of wholeness and normalcy. It is a multi-dimensional responsibility. But it’s also an amazing opportunity! It’s not just an implant—it’s giving someone’s life back to them.
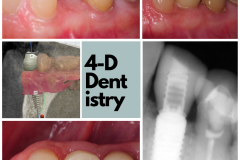
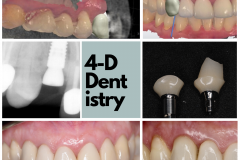
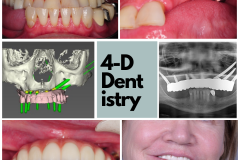
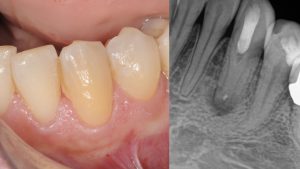 This is Nancy. She had a lower canine that had significant caries and resorption. It had to go.
This is Nancy. She had a lower canine that had significant caries and resorption. It had to go.
How are we going to proceed? Should we extract the tooth and do an immediate implant? Should we just extract it and then revisit it a couple of months later with a delayed implant? Should we graft it? How is the bone going to react? How is the soft tissue going to react?
MAYBE there’s good bone! And I say MAYBE because this two-dimensional image only shows me the height. The soft tissue has receded but it looks thick and abundant—but just how thick?
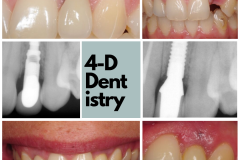
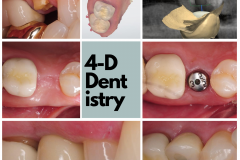
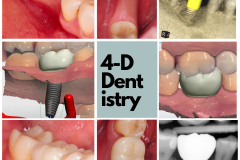
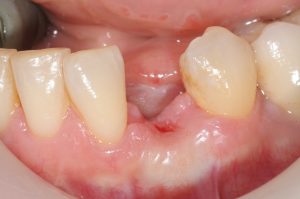 OK. The tooth was extracted and a minor site graft done to preserve and augment as much as possible. About 4 months later the patient returns and says they are ready to get their tooth back.
OK. The tooth was extracted and a minor site graft done to preserve and augment as much as possible. About 4 months later the patient returns and says they are ready to get their tooth back.
Well, that’s simple, right? Let’s put an implant, let it heal, get a crown—and voila!—you have a tooth. Yes, this looks pretty simple to me: perfectly sized space, good occlusion, thick gum tissue, and perfect bone- maybe!
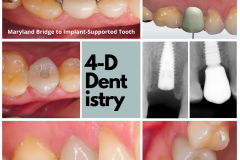
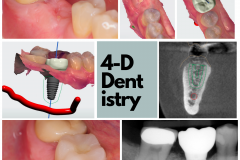
So as dentists did long ago (and many still do today), go right ahead—take a good long look at the periapical or panorex X-ray, and randomly decide on a 10-mm implant that ‘should’ work. Lets then make an incision, and put that implant in. Some may do it freehand and some may do it with a model and a surgical guide. Then, take a standard implant (hopefully that’s what they would have picked for this site) and do the drill sequence recommended by the particular implant company. Do the pilot drill, then a 2.5, 3.0, and 4.0 drill to prepare the site, and put the implant in. And then hope that it all goes well. Hope the implant is in the bone. Hope it did not hit the nerve (if this was a back tooth) or penetrate the sinus (if this was an upper back tooth). Hope it is in the right angle and position. And hope it is going to hold the crown successfully. This was life in the 2-dimensional world- lots of hoping and keeping the fingers crossed!
Next, we have to ask if it should be a single stage with a healing abutment or a two-stage delayed exposure? How does one decide that? Is it just ‘how I do it’, or what’s easier for the patient, or what takes less time, or what’s less costly? Or should the decision be based on critical biological factors, aesthetic requirements, functional needs, and tissue preservation principles? How about complications? Most complications in implant dentistry are in-fact directly related to this 2-dimensional dentistry approach and the ‘lets-fill-the-hole’ mentality.
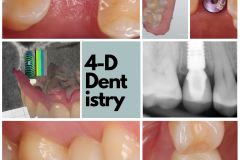
The 3-D world makes us think about things a little differently. Just how much bone do we have? And how is it changed during the implant preparation drilling process? Will the implant be in the proper vector and depth? How will it relate to the abutment and the restoration? How will those interact to support the soft tissue and papilla so we can have not only a more aesthetic outcome but also an easier-to-maintain implant? How will our implant position affect the retention mechanism, and do we even have a choice? The third dimension of our thinking and planning puts us in an entirely different orbit—more predictable, more precise, safer, easier to control—and one that is simply closer to delivering the promise to the patient. With cone beam CT scan, optical scanners, and sophisticated implant planning software, it is now easy to work in the 3-D world and take full control of the treatment. Three dimensional dentistry is no longer a luxury or done by a few with special access or knowledge to such technology. In my mind, it is now the standard-of-care and how EVERY dental implant treatment should be based on.
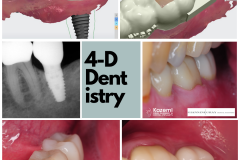
Yes, I know it’s easy to get so focused on the bone, tissue, implant, and abutments and forget that the whole reason we are doing this is to improve the patient’s life and give them back all they have lost.
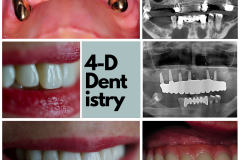
And that is what I call the 4th dimension—the remarkably happy patient who will look at their teeth every day and love them. The happy patient who is not thinking about their teeth anymore—as much as he or she does not think about their elbow. It’s just there, and it works. The happy patient who smiles openly, eats freely, and goes about their daily life the way we all like to. The happy patient that does not have to struggle removing food that gets stuck every time they eat. The happy patient that does not have to deal with loosening crowns or broken screws every month and have to take time out of their life to make yet another visit to the dentist. The happy patient that doesn’t hold back smiling because of the gray shadow of the implant reflecting through The gum tissue. The happy patient who feels whole again and can get back to work, family, traveling, socializing, and having fun. The happy patient who enjoys all the great benefits of their new tooth for many years to come. That is what I call the 4th dimension of implant dentistry.
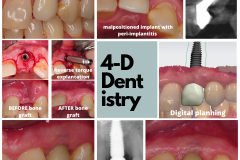
Achieving 4-dimensional results is not easy nor fast. It requires deep thinking, planning, and precise execution by an aligned team of professionals. It demands patience and an emotional engagement by not only the patient but also the treating surgeon and the restorative dentist. And yes, it is likely to be more costly. But isn’t the 4th dimension truly what patients come to us to begin with? Isn’t our responsibility to deliver the optimal treatment and not settle with mediocracy.
The road to 4-dimensional results that our patients love requires those extra efforts and sweating the details at every step of the treatment. This includes relentless diagnostics and planning, building the proper foundation, placement of the right implants in the perfect position, enhancement of hard and soft tissue at every step possible, developing biologically, functionally, and aesthetically compatible restorations, developing an effective and personal maintenance program, and perhaps the most important of all- knowing the patients’ expectations and how we can deliver the promise to meet those expectations.
And should one of my nightmares of loosing a tooth actually becomes reality, you better put me on that road.
Dr. H. Ryan Kazemi is an oral and maxillofacial surgeon in Bethesda, MD.