The Story
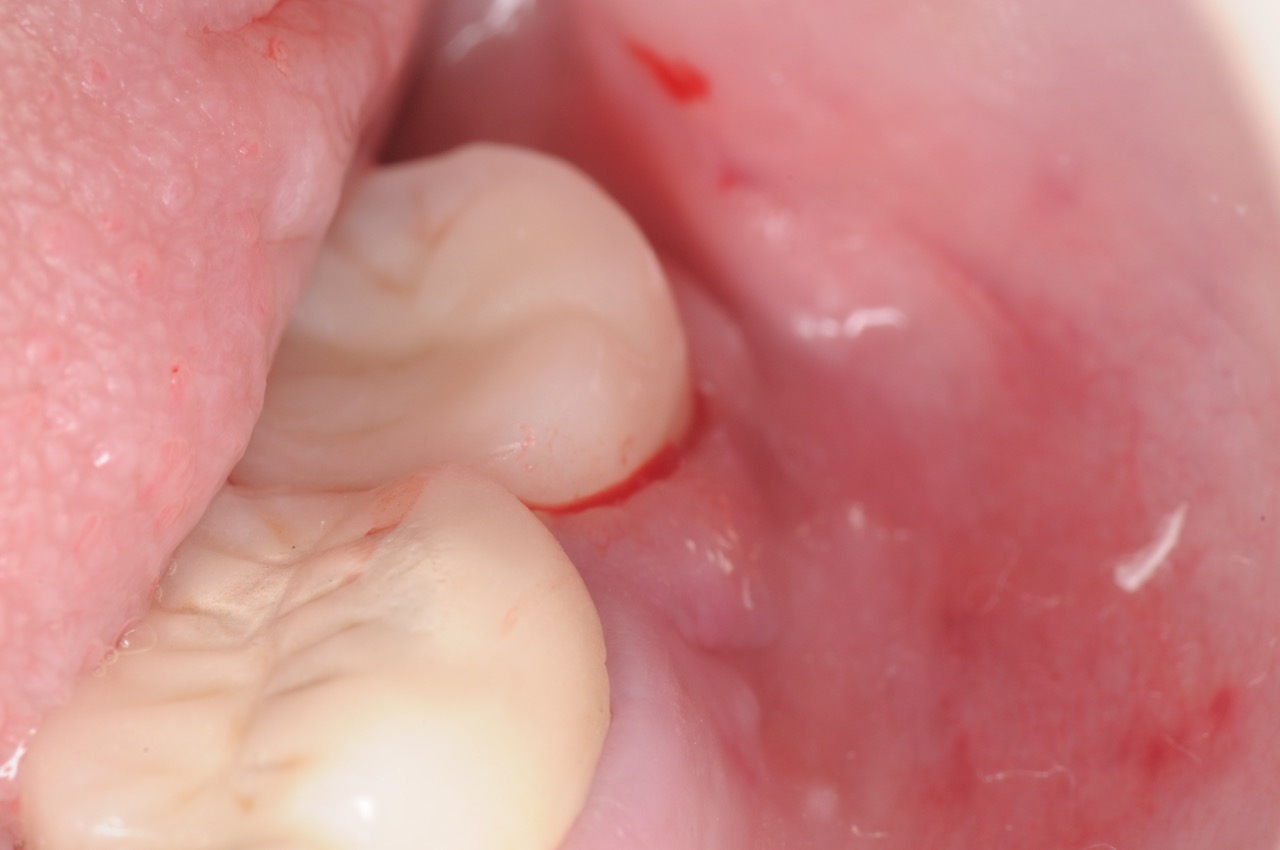
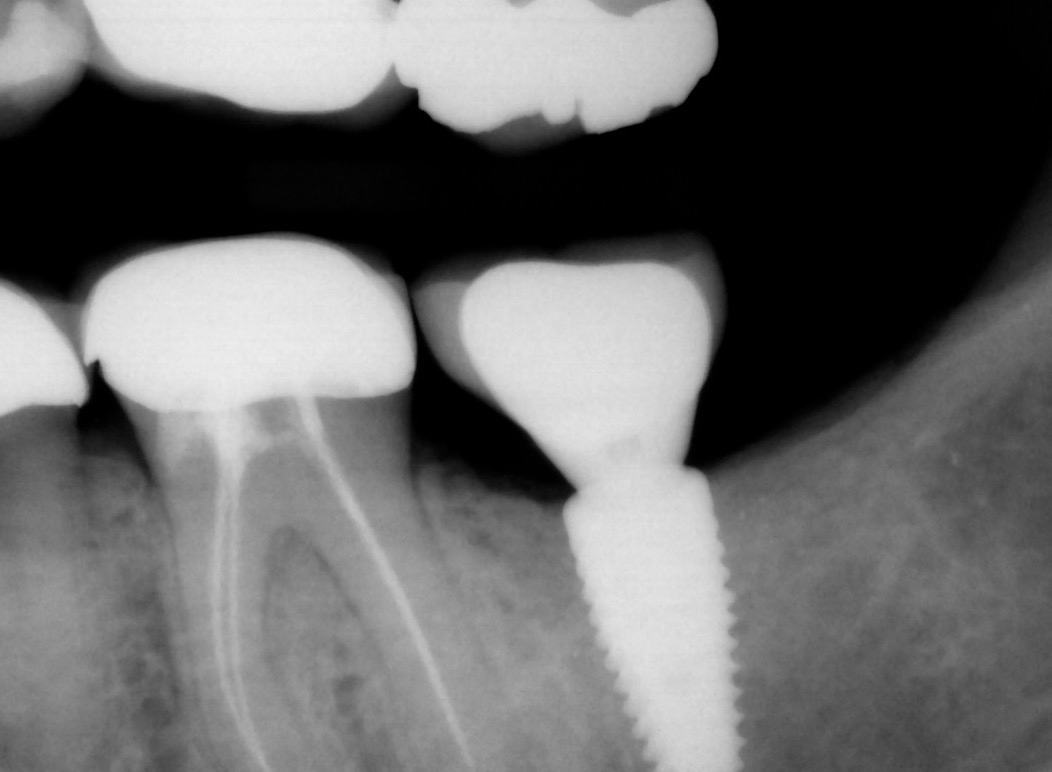
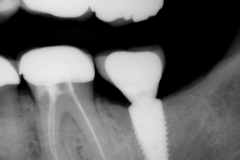
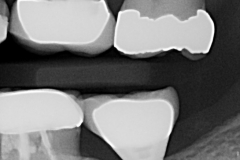
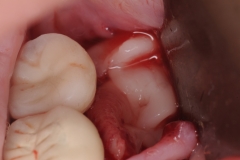
A dental implant was placed in this patient for replacement of her missing lower second molar. Several weeks after the implant was restored, she complained of increasing pain and bleeding around the gum tissue. Oral hygiene instructions were reviewed with assumption that plaque retention maybe the contributing factor to the localized inflammation. She also saw her dentist for cleaning. However neither was effective. A follow-up X-ray showed normal implant, bone and surrounding structures. Since her pain and gum bleeding did not improve, it was decided to explore the site by reflecting the gum tissue for a more direct evaluation.
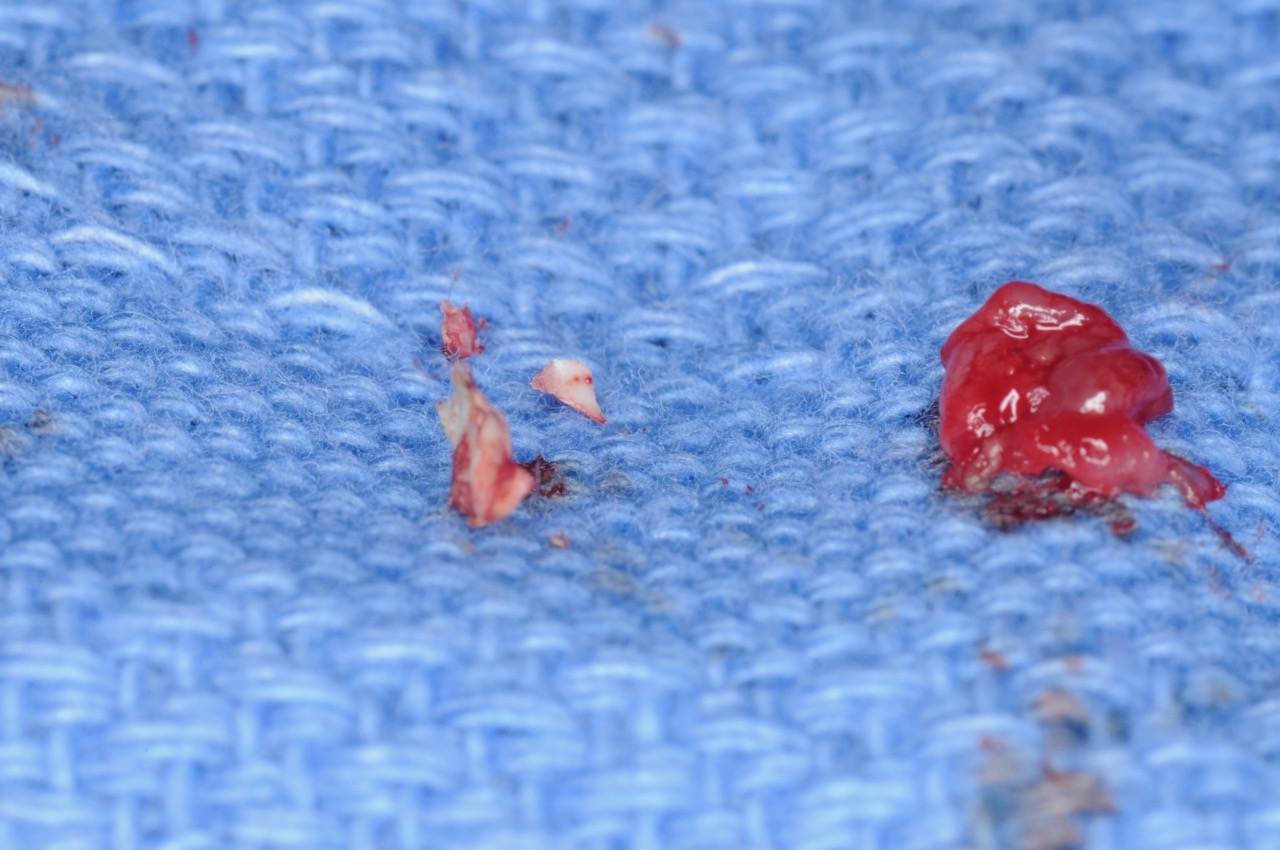
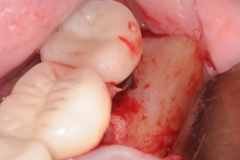
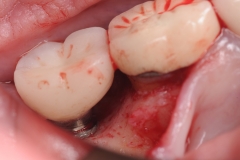
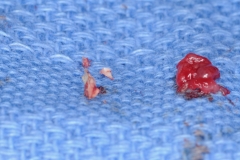
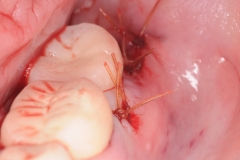
Upon evaluation, residual cement from the restoration was discovered. The cement was removed and the site irrigated to clean. Next a platelet rich fibrin membrane (derived from patient’s own blood) was placed for enhancement of the healing process. Patient was seen for follow up in 3 months and the inflammation had resolved and patient had no more pain or bleeding.
Take-Away Points
- Residual cement is very toxic to gum and bone tissues responding by formation of inflammation, granulation tissue, and infection leading to bone and soft tissue loss
- Cementation of implant crowns is certainly an acceptable approach, however screw-retained restorations are safer with regard to this risk.
- Implant crown cementation process is technically sensitive and must be done with one of several approaches that minimizes residual cement in the gingival sulcus.
- The margins of the restoration must be checked carefully and any residual cement should be removed following insertion of the crown.
- An X-ray should be taken immediately after crown placement to check for any residual cement. However, X-ray is not a definitive diagnosis for presence of residual cement. SINCE X-RAYS ARE 2-DIMENSIONAL, ANY CEMENT IN FRONT OR BEHIND THE CROWN IS NOT DETECTABLE.
Key Factors in Success
- CBCT can be helpful in localizing residual cement
- Open exploration and removal of cement followed by thorough irrigation
- Platelet rich fibrin for soft tissue healing
- Close monitoring and maintenance by Implant Care Practitioner